 If you talk to your neighbors, extended family or workmates, you’ve probably heard some COVID testing horror stories. Not so much with the test itself – though plenty of people have complained that having an oversized Q-Tip foraging around inside your nostril can be uncomfortable – but rather with delays for test results. This has most notably occurred with the high accuracy PCR tests – which at various points throughout 2020 have seen diagnostic lab backups measured in weeks, rather than days.
If you talk to your neighbors, extended family or workmates, you’ve probably heard some COVID testing horror stories. Not so much with the test itself – though plenty of people have complained that having an oversized Q-Tip foraging around inside your nostril can be uncomfortable – but rather with delays for test results. This has most notably occurred with the high accuracy PCR tests – which at various points throughout 2020 have seen diagnostic lab backups measured in weeks, rather than days.
The consequences of such lengthy delays? For one thing, it makes contact tracing weeks later virtually impossible. Also consider the financial burden on individuals & businesses (forced quarantines can mean reducing productivity to zero), as well as the health and emotional consequences (it would be nice to know whether you’re infected before visiting grandma, right?).
Speeding Test Results with Sample Pooling
When it comes to testing, one thing is abundantly clear: the sooner you receive results, the better. One solution often mentioned (and currently in use) is sample pooling.
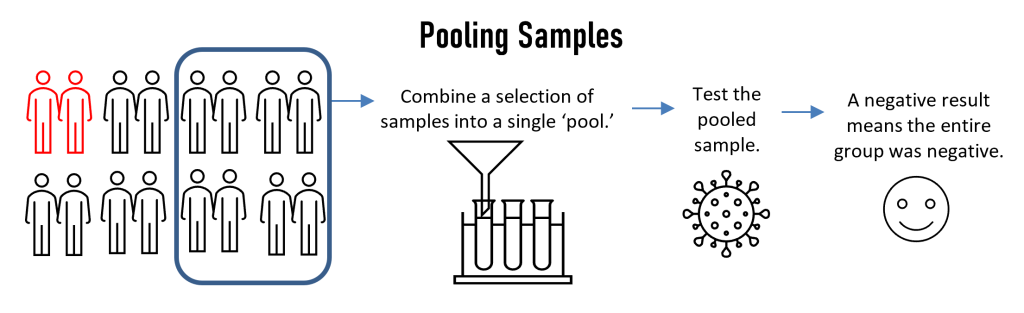
Sample pooling occurs when a lab mixes multiple samples together into a single batch (or “pooled sample”) to perform a single test on a group of samples, rather than test each individual sample. The underlying objective is simple: if the pooled sample tests negative, all of the constituent samples making up that batch are now known to be negative as well – with fewer tests needed to achieve the result.
In bioinformatics parlance, this practice is known as ‘biological averaging.’ In the field of statistics, it is known as ‘group testing.’ The concept isn’t new, by any stretch. Harvard Professor of Political Economy Robert Dorfman first described the practice in his 1943 paper, The Detection of Defective Members of Large Populations.
Sample pooling is used to decrease the overall number of tests, preserve testing supplies, and increase test throughput – thus shortening the time-to-result. (Not coincidentally, these are the key critical challenges we’ve faced with testing since the start of the COVID-19 pandemic.)
Challenges with Pooled Testing
Pool testing does have shortcomings in the detection of SARS-CoV-2. In correspondence published in The Lancet earlier this year, several additional challenges were outlined.
- Sample Dilution
One of the key challenges encountered with sample pooling is dilution. Because a number of samples are combined together, the pooled sample can have a lower, diluted viral load. This can translate to increased false negatives.
- Issues with Sample Collection & Analytical Variation
Both sample collection and analysis can experience issues with variation. On the sample collection side, there is very little supervision or consistency in the field, relying entirely on the skill of the frontline worker. The researchers who addressed this in The Lancet noted that “[t]he crucial preanalytical variable in SARS-CoV-2 testing is the amount of host RNA (detected by RNAse P). Before we adopted pool testing in our laboratory, approximately 3% of individual samples tested showed no RNAse P amplification, indicating inadequate sample collection, which was resolved on repeat sample collection.”From an analytical standpoint, it is crucial to ensure that chemical analysis lab methodologies do not introduce elements of variation. Even slight deviations from standardized workflows can have amplified consequences in a pooled sample setting.
- Inconsistent Methodologies
Another key issue pointed out in The Lancet related to the variation in sample sizes for different test kits. “Different RNA extraction kits recommend different volumes of sample, ranging from 140 µL to 200 µL … In a large pool of up to 30 samples, if we take 5–10 µL of each sample, there is every chance of missing borderline-positive single samples.”
 Advantages of Sample Pooling
Advantages of Sample Pooling
Pooling samples has been described as cost-effective, though that is not the primary motivation in our present pandemic. Rather, faster time-to-result increased testing volumes and conservation of testing supplies are the key drivers.
While pooling samples does introduce a degree (or potentially several degrees) of error in diagnosis, in the case of a pandemic it can help conserve a key resource: time.
It’s also a method that is appropriate for situations or locales in which there is low COVID-19 prevalence, thus reducing the likelihood of testing errors. Populations at low risk of infection and the testing of asymptomatic individuals, in particular, can be well-suited to pooled testing.
LabVantage LIMS and Sample Pooling
The LabVantage COVID-19 LIMS, which supports high throughput pooled sample testing, was developed to streamline SARS-CoV-2 testing workflows in order to reduce the risk of inaccuracies and speed up the testing process. By streamlining the testing workflow and creating a user-friendly ‘minimal click’ procedure, our COVID-19 platform addresses the latest guidance as well as the changing needs of healthcare and laboratory professionals.
Resources
Website Pages
LabVantage COVID-19 LIMS
White Papers
How to Manage COVID-19 Testing in the Workplace
Blog Posts
Is Your Lab Keeping Up with Rising COVID-19 Research Sample & Testing Volumes?
Press Releases
LabVantage Solutions Announces New Purpose-Built Biobanking LIMS Accelerator for Managing COVID-19 Testing
Case Studies
Overcoming COVID-19 Sample Handling Challenges with LabVantage LIMS
Employee Health and Safety in a Time of Crisis: Testing for COVID-19
Brochures
LabVantage COVID-19 LIMS Overview
Contact LabVantage
https://www.labvantage.com//who-we-are/contact-us/

